
You’re Not Alone: Finding Real Postnatal Depression Support
Postnatal depression support is available right now — and knowing where to start can make all the difference.
Quick resources if you need help today:
- Call or text 1-833-TLC-MAMA (1-833-852-6262) — National Maternal Mental Health Hotline, available 24/7
- Call or text 988 — Suicide and Crisis Lifeline for mental health emergencies
- Visit Postpartum Support International — find local support groups, therapists, and peer mentors
- Talk to your OB-GYN, midwife, or primary care doctor — they can screen you and connect you to treatment
- Call 911 if you or someone you know is in immediate danger
The weeks after having a baby are supposed to feel magical. But for a lot of moms, they feel heavy, confusing, and isolating — and that’s not a personal failure. It’s a medical reality.
More than 1 in 10 women will experience postpartum depression within a year of giving birth. And yet, so many suffer in silence, unsure if what they’re feeling is “normal” or something that needs real attention.
If you’ve found yourself crying without knowing why, struggling to bond with your baby, or feeling like you’re just going through the motions — you deserve support, not judgment.
This guide walks you through everything: how to recognize what’s happening, where to find help, and how to build a support system that actually works — for you and your family.
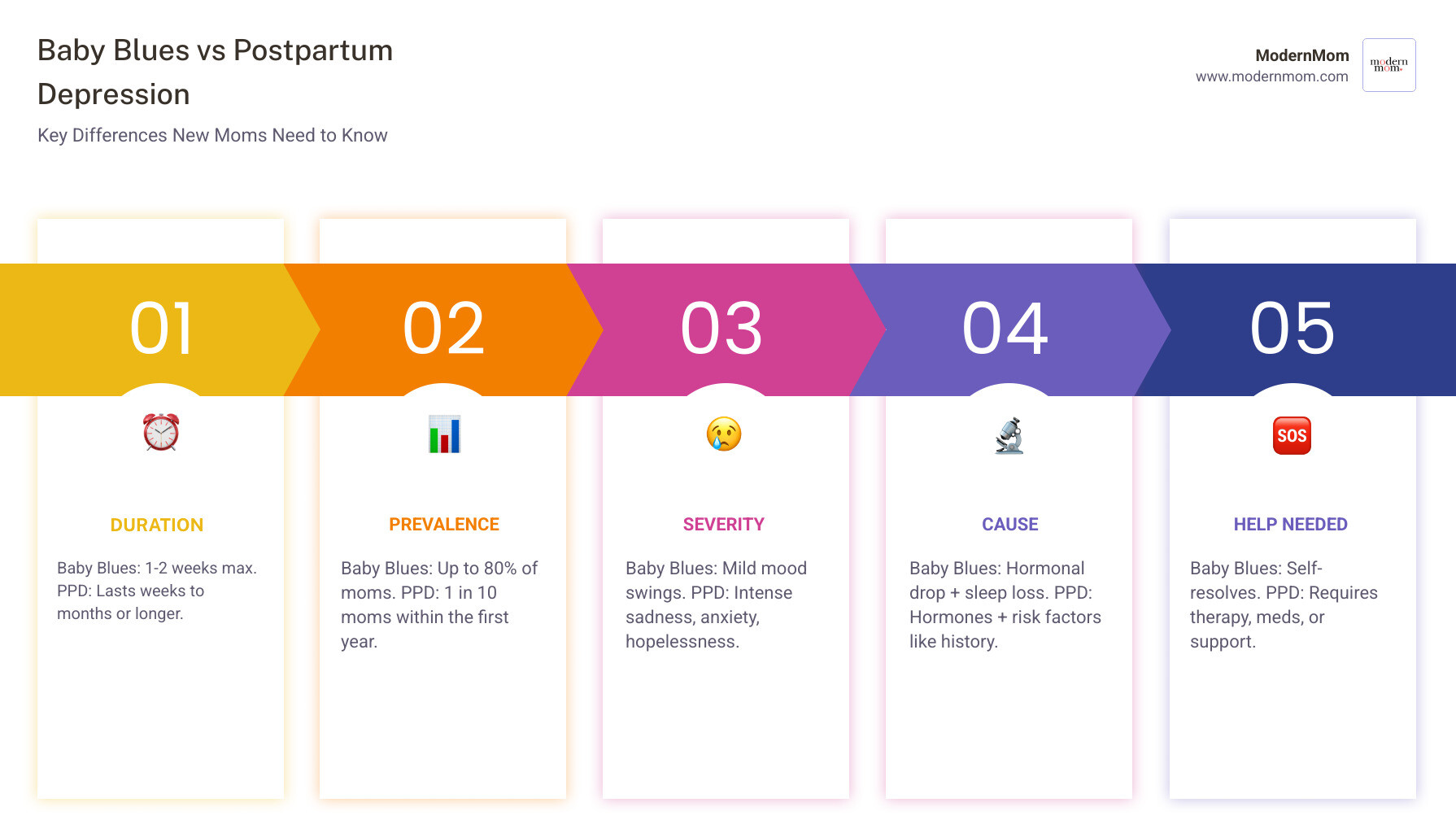
Baby Blues or Something More?
It is incredibly common to feel like an emotional wreck in the days following childbirth. In fact, up to 80% of new mothers experience what we call the “baby blues.” This usually kicks in around two to three days after delivery. You might find yourself weeping because the toast is too crunchy or feeling a sudden surge of anxiety about… well, everything.
The baby blues are primarily driven by the massive, sudden drop in estrogen and progesterone after the placenta is delivered. When you combine that hormonal freefall with extreme sleep deprivation and the shock of a new routine, it’s no wonder we feel fragile.
However, there is a distinct line between the blues and postpartum depression (PPD). The “two-week window” is the golden rule here. Baby blues typically peak and then fade away within 10 to 14 days. If your symptoms persist longer than two weeks, or if they are getting worse rather than better, it’s time to look closer.
| Feature | Baby Blues | Postpartum Depression (PPD) |
|---|---|---|
| Prevalence | Up to 80% of new moms | 10% to 20% of new moms |
| Onset | 2–3 days after birth | Anytime in the first year (often 4–8 weeks) |
| Duration | Lasts up to 2 weeks | Lasts more than 2 weeks; can last months |
| Severity | Mild; you can still function and care for baby | Severe; interferes with daily life and bonding |
| Treatment | Rest, support, and patience | Therapy, medication, and professional support |
If you are unsure where you land, it helps to learn more about the symptoms and risk factors for postpartum depression to see if your experience aligns with clinical PPD.
Recognizing the Signs and Seeking Postnatal Depression Support
Recognizing PPD isn’t always about “feeling sad.” For many of us, it shows up as “postpartum rage,” a terrifying sense of numbness, or a constant state of high alert. You might feel like you’re watching yourself through a fog.
Common symptoms include:
- Persistent sadness or “emptiness”: Crying frequently or feeling hopeless.
- Bonding difficulties: Feeling like you don’t “love” the baby the way you should or feeling disconnected.
- Intrusive thoughts: Scary, repetitive thoughts about harm coming to the baby or yourself.
- Appetite and sleep changes: Being unable to sleep even when the baby is sleeping, or having no interest in food.
- Overwhelming fatigue: Feeling a “heaviness” that makes getting out of bed feel impossible.
We know that managing new mom stress is part of the journey, but PPD is a different beast. It’s not just “stress”; it’s a chemical imbalance that requires a specific type of postnatal depression support.
When to Reach Out for Help
We often tell ourselves, “I’ll feel better once the baby sleeps through the night” or “I just need more coffee.” But if your daily functioning is impaired — meaning you can’t shower, eat, or care for your little one — you need to reach out.
If you feel worthless, excessively guilty, or like your baby would be better off without you, please know these are lies told by the depression. You can use this tool to find a health center to locate affordable care in your area immediately.
Where to Find Immediate Postnatal Depression Support
You don’t have to wait for an appointment to get a lifeline. There are incredible organizations dedicated to catching moms before they fall.
- National Maternal Mental Health Hotline: Call or text 1-833-TLC-MAMA. They offer 24/7, free, confidential support in English and Spanish.
- 988 Suicide and Crisis Lifeline: If you are having thoughts of self-harm, call or text 988.
- Postpartum Support International (PSI): This is the “gold standard” for resources. You can find Postpartum Support International resources, including specialized support groups for military moms, loss, or NICU parents.
Treatment Paths: Therapy, Medication, and Self-Care
The good news? Postpartum depression is highly treatable. Most moms find the best results through a combination of professional help and lifestyle adjustments.
1. Talking Therapies
Cognitive Behavioral Therapy (CBT) and Interpersonal Therapy (IPT) are the two most effective types of therapy for PPD. CBT helps you identify and change negative thought patterns (like “I’m a bad mom”), while IPT focuses on your relationships and the massive transition into your new role.
2. Medication
Sometimes, our brains just need a little chemical help to get back to baseline. Antidepressants (SSRIs) are commonly prescribed. Many moms worry about breastfeeding, but experts say the risk of birth defects or issues for nursing babies is very low compared to the risks of untreated depression.
3. Specialist Teams and Mother-Baby Units
In severe cases, you might be referred to a specialist perinatal mental health team. In some regions, there are even Mother-Baby Units (MBUs) where you can receive intensive treatment without being separated from your infant.
How Loved Ones Can Help
If you are a partner, friend, or family member, your role is crucial. The most important thing you can do is be specific. Don’t say, “Let me know if you need anything.” That just gives a depressed mom another task to do.
Instead, try these:
- “I’m bringing dinner at 6:00. I’ll leave it on the porch or come in and wash dishes, whichever you prefer.”
- “I am coming over to hold the baby for two hours so you can take a nap. No arguments!”
- “I noticed you’ve been having a hard time. I found a few local therapists who specialize in PPD; would you like me to help you book an intro call?”
Creating a Plan for Postnatal Depression Support at Home
We recommend building a “Home Team.” This is a group of people who have assigned roles. Maybe your partner handles all diaper changes from 8 PM to midnight so you can get a solid block of sleep. Maybe your sister is in charge of the grocery delivery.
Protecting the mother’s sleep is the #1 non-medical intervention for mood disorders. Use these tips for talking with a healthcare provider to ensure the whole family is on the same page regarding the treatment plan.
Postpartum Psychosis and Emergency Care
It is vital to distinguish PPD from postpartum psychosis, which is a rare but severe psychiatric emergency. It affects about 1 to 2 out of every 1,000 births and usually starts within the first two weeks.
Symptoms include:
- Hallucinations (seeing or hearing things that aren’t there)
- Delusions (strongly held beliefs that aren’t true)
- Extreme agitation or inability to sleep for days
- Paranoia regarding the baby
This is a “call 911” situation. It requires immediate hospitalization to keep both mom and baby safe. Organizations like Action on Postpartum Psychosis provide specialized support for families navigating this crisis.
Frequently Asked Questions about Postpartum Mood Disorders
Can postnatal depression affect fathers or partners?
Yes! About 8% to 10% of fathers experience PPD. For non-gestational parents, the cause isn’t a drop in pregnancy hormones, but rather extreme sleep deprivation, the weight of new financial responsibility, and relational stress. If the birthing parent has PPD, the partner’s risk jumps to 50%. You can read more about postpartum depression in men research to understand how it manifests differently, often as irritability or social withdrawal.
How long does postpartum depression typically last?
Without treatment, PPD can last for months or even years, potentially leading to chronic depression. However, with early intervention, many moms start feeling significantly better within a few weeks. Most episodes begin within 4 to 8 weeks of birth, but you can be diagnosed anytime in the first year.
Can PPD be prevented if I am at high risk?
If you have a history of depression or experienced PPD with a previous child, you are at higher risk. The U.S. Preventive Services Task Force recommends preventive counseling (like CBT or IPT) during pregnancy for those at risk. Building your postnatal depression support team before the baby arrives is the best defense. Review the Perinatal Depression: Preventive Interventions for clinical guidelines.
Conclusion
At ModernMom, we want you to know that struggling with your mental health doesn’t make you a “bad” parent. It makes you a human going through a massive biological and life shift.
Recovery isn’t just possible; it’s likely — provided you have the right tools and a community that holds you up. Whether it’s through therapy, medication, or simply a group of fellow moms who “get it,” help is within reach.
Seeking help isn’t a sign of weakness; it is the ultimate act of strength for you and your baby. For more tips on navigating the beautiful, messy journey of motherhood, visit ModernMom for more parenting and wellness resources.
The post How to Find Real Help During the Postpartum Period appeared first on ModernMom.

